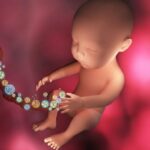
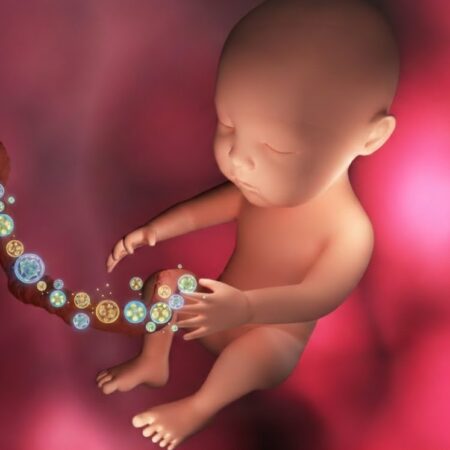
Type 2 diabetes (T2D) is a significant global health challenge, affecting 11.1% of adults worldwide [2025 International Diabetes Federation (IDF) Diabetes Atlas]. Parasitic helminths—multicellular worms that have co-evolved with humans—continue to infect over 250 million people, mainly in tropical regions.
New clinical studies suggest an inverse relationship between these parasitic infestations and T2D, indicating that helminth colonisation may be protective against insulin resistance and metabolic syndrome.
The Aftermath of Infection Eradication
According to the ‘hygiene hypothesis’, eradicating helminths in high-income countries has limited morbidity in humans. However, this correlates with a sharp rise in ‘Western’ diseases, including autoimmune disorders and metabolic dysfunction. Although parasites are often linked to negative outcomes, such as growth retardation and anaemia, they have adapted to survive by balancing their host’s immune response and metabolism. This long-term coexistence suggests that the ‘silent majority’ of low-level infections may affect global metabolic health.
Mechanisms of Metabolic Influence
Parasites influence insulin signalling through complex immunological and metabolic pathways:
Immune Modulation: These worms cause an infection that drives a shift from a pro-inflammatory T helper 1 (Th1) response to an anti-inflammatory Th2 response, characterised by the cytokines interleukin (IL)-4, IL-5, and IL-13. This alteration promotes the accumulation of ‘alternatively activated’ (M2) macrophages and eosinophils in white adipose tissue (WAT).
Adipose Tissue Homeostasis: These type 2 immune cells protect against obesity-driven inflammation, a primary cause of insulin resistance. Furthermore, these cells can promote the ‘beiging’ of white fat—conversion of white fats into brown fats—that increase energy expenditure and dissipate energy as heat.
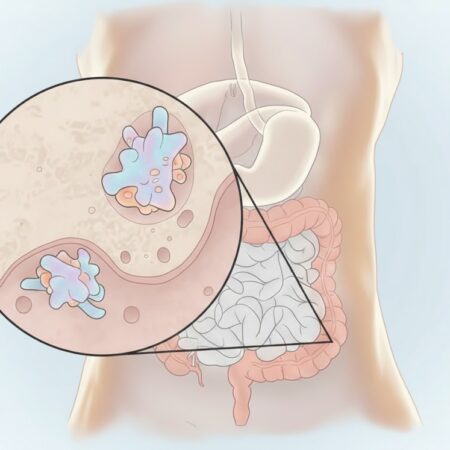
Glucose and Lipid Regulation: Evidence suggests that helminths limit intestinal glucose absorption by inhibiting sodium-linked glucose transporters (SGLT1) and insulin-dependent transporters (GLUT2). Some species also hijack host lipid resources for their own egg production, effectively lowering total cholesterol and triglyceride levels.
Clinical and Epidemiological Evidence
Population-based studies provide compelling data regarding this protective effect. In a cross-sectional survey conducted in rural China, individuals with a history of schistosome infection exhibited lower Body Mass Index (BMI), waist circumference, fasting blood-glucose, and HbA1c levels. Similarly, a study in the Lambaréné region of Gabon found that Schistosoma haematobium infection was associated with significantly improved lipid profiles in overweight individuals.
Recent clinical trials show progress from observation to intervention. A double-blinded, placebo-controlled trial involving 40 adults at risk of T2D assessed the administration of Necator americanus (hookworm) larvae. The study found that fasting blood-glucose levels and insulin resistance declined in both treatment groups (those receiving 20 or 40 larvae) after one year. Additionally, the group receiving 20 larvae showed a reduction in BMI at the end of two years after intervention.
Clinical Impact and Future Directions
The clinical impact of these findings is profound, potentially redefining management strategies for metabolic diseases.
Current research focuses on harnessing helminth-derived excretory-secretory (ES) products—heterogeneous mixes of proteins and lipids—as novel therapeutic agents. These molecules mimic the immunomodulatory power of a live infection without the associated risks of morbidity or transmission.
While significant cultural and regulatory barriers persist, elucidating the interplay between parasites and host metabolism opens promising therapeutic avenues. If successful, helminth-derived treatments could become a biological method to counteract the chronic low-grade inflammation that underpins the global diabetes epidemic.
Keywords: helminth therapy, insulin sensitivity, type 2 diabetes, metabolic syndrome, hygiene hypothesis, human parasites, immune modulation.
Suggested Reads:
1. Guigas B, Molofsky AB. A worm of one’s own: how helminths modulate host adipose tissue function and metabolism. Trends Parasitol. 2015 Sep;31(9).
2. Sridhar GR, Botta S, Lakshmi G. Can parasites influence insulin signaling and development of diabetes mellitus? Acad Biol. 2026 Jan 5;4. Available from: https://doi.org/10.20935/AcadBiol8088.