Type 1 diabetes (T1D) – a chronic autoimmune condition characterised by the destruction of pancreatic β-cells, causes life-long insulin dependence. While the disease is increasing globally, the earliest biological triggers have remained elusive. The previous hypothesis that T1D precipitates from an autoimmune attack is already underway.
Recent research published in Nature Communications reveals that the inflammatory pathway leading to T1D commences during pregnancy. The study draws from the Swedish population-based All Babies in Southeast Sweden (ABIS) birth cohort of 16,683 infants and identifies proteomic markers present at birth that can predict the disease with high accuracy years before a clinical diagnosis.
Identifying Risk in the Womb
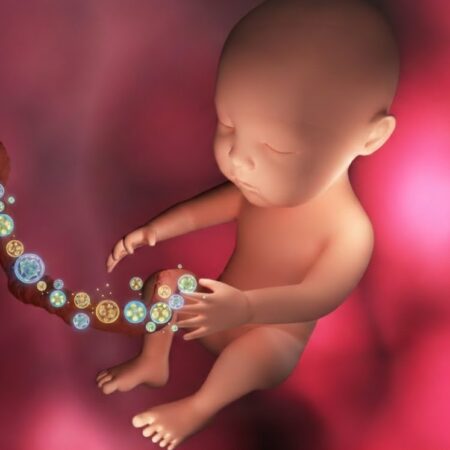
New experiments suggest that the biological foundations for T1D are established during the prenatal period.
Researchers identified significant differences in protein abundance between children who later developed T1D and those who did not—by analysing cord blood through Olink proteomic profiling.
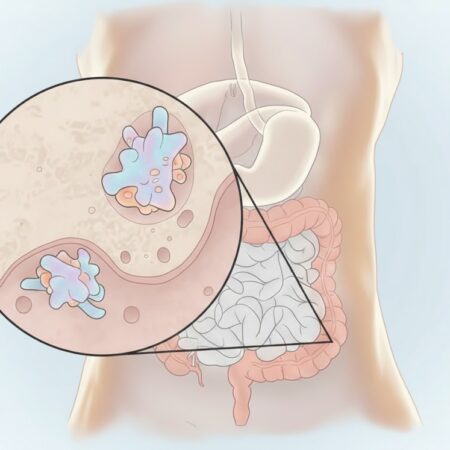
These proteins are primarily involved in innate immunity, neutrophil migration, and tissue remodelling, suggesting that β-cell vulnerability begins in utero.
Risks and Long-term Neonatal Outcomes
Prenatal risk factors are also implicated in their association with future T1D in the offspring. These include maternal infections such as the stomach flu, use of certain medications like antibiotics and psychotropics, and even significant prenatal stressors or severe life events. Furthermore, the study found that environmental toxins, specifically perfluoro-octane sulfonate (PFOS), correlate with inflammatory proteins in cord blood. Hence, low-level environmental exposure during pregnancy may subtly modulate the neonatal immune system.
The findings highlight how prenatal and early life events impact long-term health trajectories and have profound implications for neonatal care. Children born through caesarean sections had a higher risk of future T1D and showed significant correlations with at least 24 different inflammatory proteins in cord blood. In addition, the ones diagnosed with T1D were significantly more likely to have been placed in a paediatric ward or newborn care unit immediately after birth.
Novel Neonatal Biomarkers
Traditionally, T1D risk is assessed through HLA genetic screening and the monitoring of islet autoantibodies. This research identified two specific proteins, HLA-DRA and iduronate 2-sulfatase (IDS), as the most predictive markers at birth.
Elevated levels of these proteins in cord blood reflect an overactive antigen expression and altered lysosomal activity, which may predispose infants to early β-cell stress.
The study demonstrated that proteomic analysis at birth can predict T1D, independent of a genetic risk. Using machine learning models, specifically eXtreme Gradient Boosting (XGBoost), researchers achieved a high predictive accuracy with an area under the curve (AUC) of 0.89.
The results suggest that a non-invasive proteomic screen at birth could identify at-risk infants more effectively than the current genetic methods. The predictive power of these proteins extends beyond HLA genotypes. Thus, the novel biomarker can identify T1D risk in those without a known family history of the disease.
Early Detection – for T1D Prevention
This discovery may encourage early screening and foster a shift from reactive to proactive medicine. By the time childhood islet autoantibodies are detected, the inflammatory attack on the pancreas is already advanced. Identifying disruptions at birth opens a critical “window for prevention”.
Early detection will allow clinicians to monitor at-risk infants more closely. This will facilitate deploying interventions to reduce inflammation and protect β-cells before the autoimmune process becomes irreversible.
As neonatal care becomes more patient-centric, integrating proteomic screening could delay or even prevent the onset of insulin dependence in thousands of children globally. While further research is needed to generalise these findings across different populations, the ABIS study provides a robust foundation for a new era of prenatal and neonatal preventative care.
Keywords: Type 1 diabetes, neonatal screening, prenatal health, proteomics, inflammatory markers, birth cohort, autoimmune disease prevention, beta-cell protection, cord blood analysis, HLA genetic risk, ABIS study, pregnancy health, clinical biomarkers.
Suggested Read:
Ahrens AP, Dias R, Hyötyläinen T, Orešič M, Triplett EW, Ludvigsson J. The inflammatory path toward type 1 diabetes begins during pregnancy. Nature Communications. 2026 Jan 7.